|
| Making an at-chest supplementer is easy and cheap. |
Note that this post is not medical advice. I am sharing here what I have learned through personal experience. If you are concerned about your baby's health, seek help from a doctor.
Using an at-chest (at-breast) supplementer is a great way to feed your baby if you are unable to produce all of the milk he or she requires. This method is completely supportive of the nursing relationship, and does not involve your baby latching on to any artificial nipples, such as bottle nipples. As wonderful as it is, this kind of supplementer can be brutally hard to use at first. I've been using one for over eighteen months, so I'll share some tips!
First, let me explain what it is. All the different versions consist of a container to hold the supplement and a long, narrow tube. One end of the tube goes into the supplement, and the other end is placed right by your nipple. Your baby latches onto both the tube and your nipple simultaneously, drawing supplement from the container and getting all the milk that you are producing, too.
What's great about it? Using an at-chest supplementer allows you to do all feedings at your own chest. This is amazing for your nursing relationship and all the bonding that comes with it. It's also important for promoting normal jaw development in the infant - the physical action of chestfeeding develops a baby's muscles differently than bottlefeeding does. Using the supplementer helps you produce more milk, too, because even at times when your baby is only receiving supplement and you are not producing any milk, your chest tissue is being stimulated to make more. For those who produce little to zero milk, using the supplementer makes it possible to still have a nursing relationship.
How do I get one? You can buy a commercial supplementer, or you can easily and cheaply make your own. I prefer the homemade kind, so that's what I'll describe first. You can use any baby bottle to hold your supplement. Get gavage tubes from a pharmacy, or in bulk from a medical supply store. The kind to look for is 5 French (that's the diameter), 36 inches in length. You might want a tube with a bigger diameter if your baby has a weak suck, a complication of some conditions such as cleft palate or prematurity. Using a shorter tube is super irritating because it forces you to hold the supplement container so close to your baby's mouth (who has enough hands to do all that?!). Cut off the extra plastic bits, if there are any, on one end of the tube. The other end will be closed and rounded and will have two or three holes just before the tip - I cut off this part too because otherwise the supplement doesn't seem to come out easily. Some don't do this because they believe that cutting this end makes the tube sharp (we never experienced a problem with this). Thread one end of the tube through the bottle nipple (expand the opening of the nipple with a knife if required) so that it is sitting in the supplement. To clean the tube after use, just suck some hot water through it.
Do not boil this kind of tube - it is not made from materials designed to withstand such a hot temperature.
The main difference between the homemade and commercial systems is cost. The Lact-Aid is $48.75 or $62.50, depending on whether you get the deluxe or standard model. The Supplemental Nursing System (SNS), made by Medela, was $42.99 on Amazon when I checked at the time of writing. It should be noted that
Medela is a company that violates the World Health Organization's code on the marketing of bottles and artificial nipples. Unfortunately, its product name, SNS, is often incorrectly used as a generic name for a supplementer. You can make your own supplementer for the cost of any baby bottle and nipple and a $5.00 gavage tube. If you use this system in the long-term, you will end up spending a fair bit on tubes. They can be bought in bulk for about $1.00 a piece, and most people replace them once per week (or when they get too stiff to use) - so, you could spend $52 on tubes if you use the homemade supplementer for one year. I've been told by several people who used an SNS or Lact-Aid for over a year that both systems hold up very well to wear and tear and rarely need replacement parts.
With both the SNS and the Lact-Aid, the supplement container hangs around your neck. I like my homemade version because I can put the container down beside me on a table or hold it between my knees - I hated the idea of something relatively heavy dangling from my neck. I also like being able to have a decent amount of supplement on hand. The containers of the SNS (re-usable) and Lact-Aid (disposable bags) are smaller than most baby bottles. My number one reason for using my homemade version is that it is simpler - it has only three parts (bottle, nipple, and tube).
 |
| Moulding the chest tissue and positioning the tube |
How do you actually use this thing?? Some people latch the baby on first, and then sneak the tube in through the corner of the baby's mouth by moving a bit of breast tissue gently out of the way. This never worked for me. I have so little chest tissue that if I moved any part of it, my baby would lose his grip immediately. A downside of this method that a friend of mine learned the hard way is that it may become impossible to sneak the tube into your baby's mouth once he or she has teeth getting in the way.
There's a lot to have to juggle between latching your newborn and placing a tube.
This is how I do it: I get my baby in position and latch him first without the tube (otherwise he gets too antsy waiting for me to have everything ready). Then I take the end of the tube and get it near the end of my nipple. I briefly un-latch my baby. I use my thumb and middle finger to mould my chest tissue into a shape that my baby can latch to, and use my index finger to position the tube so that the end of it is in line with the tip of my nipple. The tube comes from above my nipple so that it points to the roof of my baby's mouth when he latches. I slip my index finger out of the way just as he is latching on and then I hold the tube in place for an extra second or two until the supplement is flowing up the tube. Some people tape the tube to their chest, but this didn't work for me. The tube would always flip in the wrong direction when I tried to mould my chest tissue for my baby to latch.
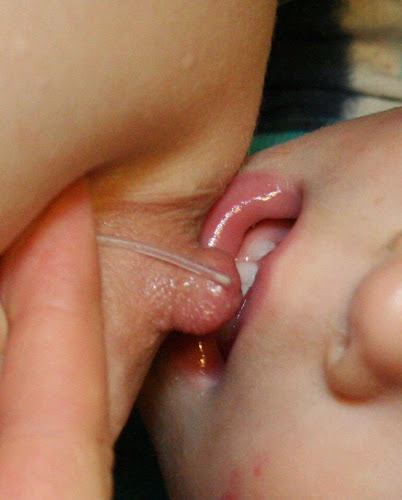 |
| About to latch |
Using a supplementer is initially very challenging. I couldn't position it on my own for the first two weeks! My partner had to help me with every single feeding until I developed this method of doing it on my own. It helped when my baby's latch became stronger. Nowadays, at eighteen months, I don't even think about it. My baby latches himself on, and I know exactly where the tube needs to go so that the supplement will come up easily.
Have you used a supplementer? Do you have any additional tips to share that we should know about?