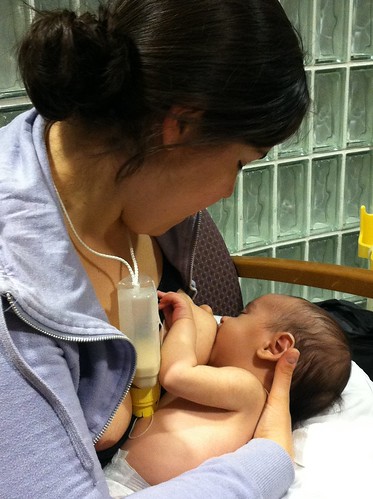
This beautiful, eloquent post by Lisa van den Hoven gives us a few straight truths about milksharing and helps put it all in perspective. What does it really mean to give your milk to a "stranger"? What exactly does milksharing look like?
Many thanks to Peaceful Parenting for hosting Lisa's piece in World Milksharing Week's Blog Carnival.
Lisa and her little one, who shares her milk.
Let’s talk about that controversial thing called milksharing. The facts, as I understand them, are that Emma Kwasnica, with the help of many other like-minded people, launched a global network, through Facebook, called Human Milk 4 Human Babies. The aim of the network is to connect moms who need milk for their babies, with other moms, who have milk that they can share. This was about meeting a need.The World Health Organization’s position on infant feeding is that if, for some reason, a mother is not able to feed her own baby, milk from another human mother is a better alternative than formula. Milk banks do exist that could theoretically meet this need, but there are some problems. First, there are very few of them, so the milk that they do have to give gets prioritized to very sick or premature babies - the infants that desperately need the milk. Second, milk bank milk is almost always pasteurized, which turns human milk from the living miraculous stuff that it is, into dead milk, losing much of its value. Finally, it costs money to access the milk of many milk banks. So even if your baby is among the few that make the cut, and you are happy to accept pasteurized milk, you may still have to come up with the cash to cover it.
The medical community is aware of how difficult it is to access human milk when you need it -- this is why they do not often advise mothers to try this option. Instead, supplementing with formula is quickly suggested. I do not intend to go into why this is such a poor choice here. Suffice it to say there are mothers out there for whom supplementing with formula is not an option that they are comfortable with. So, do they have to? Is there no other choice?
Let’s be realistic: human milk is not a scarcity! Many mothers have ample supply for their babies, and then some. Some women struggle with oversupply! It is also a vastly renewable resource - empty breasts will fill themselves again and again. It should not be so hard to connect people who need milk to people who have milk to give. And it turns out, it isn't. But fear is alive and well.
When a group of parents decided they were done waiting for the medical community to fix this problem, and opened up a way for donors and recipients to easily match up, there was massive push back. It must not be safe, right? People could have disease! You never know what they might be smoking in their spare time... That's just gross, anyway.
Really, all of the arguments against this wonderful, simple milksharing solution to a common problem sound the same to me as razor blades in apples at Halloween. I doubt that there are all kinds of sadistic, lactating weirdos out there, masquerading as concerned moms, handing out drug-laced human milk donations just for jollies.
Here are a few facts:
Human Milk 4 Human Babies donors do not charge for their milk. There is nothing to be gained by donation, save the truly awesome global village feeling that you are helping to feed another's child.
Milksharing is done person to person. That means you meet that person you are getting milk from. You ask questions. You go to their house and meet their family. And you decide whether or not your baby eats that milk. You decide.
This is not a new idea. Wet nursing has been done throughout human history.
And, now a confession: My name is Lisa, and I have donated my milk to a stranger.
Based on the oh-so-educated comments that I read elsewhere on the internet, a common reaction to this is, “Omigosh! Weirdo!” or maybe just, “Yuck. I could never do that.”
But before you decide how you feel about informal milksharing, read just a teensy bit more.
I say I gave my milk to a stranger, in that this was someone that I initially met over the Internet. But when she sat in my living room, with her husband and new son, and we chatted while my similar-aged daughter cooed in her swing nearby, stranger was not the word I would have used to describe her. It actually didn’t feel strange at all. We were just two moms. She had a problem, and I was in a position to help her out, in a meaningful way. I am so glad she was not too scared to accept my help. Donating milk was hugely rewarding for me, even renewing much of my faith in the spirit of community.
If only more moms were not scared milk-less. We don't always need to turn to the authorities to fix our problems. Sometimes, with a little courage, we can find our own solutions.
Lisa is Mom to two, wife to one, and lives in Winnipeg, Manitoba, Canada. She loves being busy in her local, gentle parenting community, and blogs occasionally at Swirls and Swings.
Related Reading:
Breastmilk Donation Page [This page was created prior to milksharing communities existing as they do in 2012. For many years peaceful parenting served, in part, to connect mothers with donors locally via email, phone and community networking. Today, thanks to the new mother-to-mother milksharing set-ups, we hear from far fewer who don't already have their needs met or connections established.]
Joshua's Story: Why I Choose Another Mother's Milk
Joshua's Story: Why I Still Choose Another Mother's Milk
Human Milk for Human Babies After Japan Tsunami
Reasons Not to Send Formula or Human Milk to Haiti and Other Disaster Locations
TIME Reports on New Global Milksharing
Delaney Rose: 6 Months of Milksharing
A Modern Day Wet Nurse
From Despair to Donation: A Mother Loses Her Baby and Shares His Milk
Showing posts with label Human Milk 4 Human Babies. Show all posts
Showing posts with label Human Milk 4 Human Babies. Show all posts
28 Sept 2012
27 Sept 2012
Overcoming Difference Through Milksharing
I've been having tons of fun reading and posting everyone's pieces for World Milksharing Week's Blog Carnival. After musing on it forever, I finally wrote my own today, about finding my place in the milksharing community.
I am a transgender man. I am in a gay relationship. I breastfeed my kiddo.
And I can tell you right now that I feel a deeper connection to our Mormon and Mennonite milk donors than I do to many of my other friends and community.
My past experiences as an LGBT person encountering religious folk have generally not been pleasant. Among many other comments, a Muslim friend once told me that being gay is worse than committing murder (I hadn't yet transitioned at the time), and a Christian noted that queer people burn in hell forever. My partner and I posted on Human Milk 4 Human Babies that we were a gay couple looking for milk for our baby, and assumed that LGBT-friendly donors would self select. We hoped that others would remain silent.
When I first realized that one of our milk donors, we'll call her Sherry, was Mormon, I was totally shocked that she would want anything to do with us. We had received her milk through a friend, and I thought that perhaps the original donor just didn't know much about us. We met for the first time a few days later, and Sherry gushed over our ten day old boy. In fact, I believe she said to him something like, "You make my uterus ache! Holding you makes me want another baby."
At that moment, I realized that Sherry and I had much in common. We both love holding babies, we are both attachment-minded parents, and we both really care about the health of babies - all babies. Sherry's milk maintained my son's normal gut flora on his fifth day of life, while a feeding of formula would have altered it, for the worse, for weeks to come.
Some Christian donors have told us that they don't understand everything about who we are, but they are open to learning, and they have a whole lot of respect for our commitment to breastfeeding and human milk. I am learning that there is great variety amongst individuals' religious paths. Not every Christian I meet is like the woman who once hurled the phrase "Jesus loves you" at me as if it was some kind of insult.
Outside the milksharing community, I often get comments like, "You're sure letting the baby run the show, aren't you? You know he would be fine. Formula isn't evil. It's ok to cry." I am simply responding to my son's needs - to be picked up, to nurse, to have human milk. I feel misunderstood, defensive and embarrassed when someone criticizes my parenting in this way. I know that I have done my own reading about everything from the risks of formula feeding to the effect of excessive cortisol in the brain of a baby who is left to cry. It's not that I lose confidence in what I'm doing when I listen to such remarks, but I very quickly feel that I am an unwelcome, "other" kind of person ("other" being a word I had previously associated only with being transgender in a cisgender world.)
A few years ago, I would never have guessed that my family's strongest, most supportive parenting community would include people who are aligned with religions that have deeply conservative threads. The milksharing community is incredibly diverse in terms of ethnicity, family structure, sexual orientation, financial status, religion, and language - it is expanding rapidly all over the world.
When one parent goes to the trouble to express and store her milk, and she posts on a social network to find someone to give it to so it won't go to waste, we know that she values human milk. When another parent responds to her post and drives across the city to pick up that milk rather than buying a can of formula from the corner store, we know that he or she prioritizes normal infant nutrition. Donors and recipients meet on the common ground of good health. It is that simple.
I am a transgender man. I am in a gay relationship. I breastfeed my kiddo.
And I can tell you right now that I feel a deeper connection to our Mormon and Mennonite milk donors than I do to many of my other friends and community.
My past experiences as an LGBT person encountering religious folk have generally not been pleasant. Among many other comments, a Muslim friend once told me that being gay is worse than committing murder (I hadn't yet transitioned at the time), and a Christian noted that queer people burn in hell forever. My partner and I posted on Human Milk 4 Human Babies that we were a gay couple looking for milk for our baby, and assumed that LGBT-friendly donors would self select. We hoped that others would remain silent.
When I first realized that one of our milk donors, we'll call her Sherry, was Mormon, I was totally shocked that she would want anything to do with us. We had received her milk through a friend, and I thought that perhaps the original donor just didn't know much about us. We met for the first time a few days later, and Sherry gushed over our ten day old boy. In fact, I believe she said to him something like, "You make my uterus ache! Holding you makes me want another baby."
At that moment, I realized that Sherry and I had much in common. We both love holding babies, we are both attachment-minded parents, and we both really care about the health of babies - all babies. Sherry's milk maintained my son's normal gut flora on his fifth day of life, while a feeding of formula would have altered it, for the worse, for weeks to come.
Some Christian donors have told us that they don't understand everything about who we are, but they are open to learning, and they have a whole lot of respect for our commitment to breastfeeding and human milk. I am learning that there is great variety amongst individuals' religious paths. Not every Christian I meet is like the woman who once hurled the phrase "Jesus loves you" at me as if it was some kind of insult.
Outside the milksharing community, I often get comments like, "You're sure letting the baby run the show, aren't you? You know he would be fine. Formula isn't evil. It's ok to cry." I am simply responding to my son's needs - to be picked up, to nurse, to have human milk. I feel misunderstood, defensive and embarrassed when someone criticizes my parenting in this way. I know that I have done my own reading about everything from the risks of formula feeding to the effect of excessive cortisol in the brain of a baby who is left to cry. It's not that I lose confidence in what I'm doing when I listen to such remarks, but I very quickly feel that I am an unwelcome, "other" kind of person ("other" being a word I had previously associated only with being transgender in a cisgender world.)
A few years ago, I would never have guessed that my family's strongest, most supportive parenting community would include people who are aligned with religions that have deeply conservative threads. The milksharing community is incredibly diverse in terms of ethnicity, family structure, sexual orientation, financial status, religion, and language - it is expanding rapidly all over the world.
When one parent goes to the trouble to express and store her milk, and she posts on a social network to find someone to give it to so it won't go to waste, we know that she values human milk. When another parent responds to her post and drives across the city to pick up that milk rather than buying a can of formula from the corner store, we know that he or she prioritizes normal infant nutrition. Donors and recipients meet on the common ground of good health. It is that simple.
25 Sept 2012
A Story of Peace and Healing

This touching, personal milksharing journey was submitted by Diana Cassar-Uhl, IBCLC and blogger at Normal, Like Breathing.
If you’ve visited my blog before, you know that I believe in human milk for human babies, and I have a deep understanding and empathy for those mothers who can’t or choose not to breastfeed their babies, for whatever reason. This week, World Milksharing Week, offers a perfect opportunity to highlight a beautiful story of love and healing, of generosity and peace that have been made possible by the gifts of milk donors.
First, be sure to check out this comprehensive report about mother-to-mother milksharing, by Amber McCann, IBCLC, and, from the International Breastfeeding Journal, Milk sharing: from private practice to public pursuit.
Stephanie was heartbroken after her first baby, Isaiah, was born and she realized she couldn’t make enough milk to meet his nutritional needs and sustain his growth. A condition called mammary hypoplasia/insufficient glandular tissue (IGT) made it so that she could only produce about 4 ounces of milk each day; she had to supplement Isaiah’s intake with something other than her own milk, and at the time, commercially-prepared baby milk (formula) was, as far as she knew, her only option. “I knew there was such a thing as donor breastmilk, but I thought it was only for sick babies,” Stephanie explains. “We supplemented with just about every formula under the sun,” Stephanie recalls. Isaiah had an undiagnosed cow’s milk protein intolerance; watching him suffer, and knowing the cow’s milk-based formula was likely to blame was very difficult. Stephanie felt as if her body had failed her baby, and every day, every supplemental feeding, the pain of this feeling was new. “When I was pregnant again, I heard about mother-to-mother milk sharing on the IGT support page on Facebook and immediately knew this was what I wanted to do.”
 |
| Stephanie breastfeeding baby Elliot |
 |
| The gift of donated milk fills more than the freezer, it fills the hearts of both the donor and recipient families. |
Shelly lives an hour away from Stephanie, in southern Maine. The first time she traveled to pick up the milk Shelly was donating to her and her baby, Elliot, Stephanie had to ask friends to loan her coolers - six of them - so they’d be able to keep all of the milk cold on the trip home. “I couldn’t believe it! Our 7 cubic-foot freezer was nearly full after that first donation!” In her two trips to Shelly’s house, Stephanie acquired over 3000 ounces of milk.
The milk wasn’t all Shelly shared, however, and it wasn’t the only thing Stephanie and Elliot gained. The two families became friendly, the dads enjoying each other’s company while the moms gathered Shelly’s milk and supervised their little ones, who, at the last pick-up, were delighted by an impromptu play-date. “The connection was immediate, we clicked,” Stephanie says. “It felt right. The thought that a mother — and her child — would care so much as to aid us in our goals is truly heartwarming. The generosity that she has bestowed upon us leaves me in tears every time I think about it. We could never be grateful enough for the hearts of these mothers.”
 |
| Shelly with her children, left, with Stephanie and Elliot, right, at the last milk pick-up |
Even after that year goes by, Stephanie knows that Shelly and the other mothers who have assisted with her breastfeeding journey will hold a permanent place in her family’s heart. She hopes her friendship with Shelly will be enduring as their children grow up and breastfeeding becomes a memory for both families. Stephanie says “I will forever be indebted to Shelly and the other mothers who have donated their milk, time, and love. Their giving hearts have changed my life. Shelly has helped us defy all odds. She is amazing and I am blessed having her in my life. I will never take for granted all that she has done for us. Calling her a milk donor will never be honorable enough … these moms are superheroes.”
If you have milk to donate, you have options. Milk
banks in the United States are always eager to accept milk donations,
but certain requirements, such as the age of your baby, must be met. Read more about donating to an HMBANA milk bank.
If you’d like to share your milk with a mother and baby
in need and you don’t meet the requirements for donation to a milk
bank, or you would prefer a mother-to-mother arrangement, visit any of
the milksharing websites that were linked above. Be sure to adequately
inform yourself and examine the risks and the benefits of feeding your
baby donated human milk, and determine whether the benefits outweigh the
risks for your situation and your baby.
21 Sept 2012
Supporting Families in Milksharing as an International Board Certified Lactation Consultant
This year's World Milksharing Week Blog Carnival includes posts by a wide variety of individuals, including donors, recipients, activists, academics, authors, and health professionals. I am thrilled to present this piece by Amber McCann, blogger and International Board Certified Lactation Consultant, about why she, as a health care provider, supports milksharing. She explains what people like her can do to help their clients make informed choices in milksharing, an area that many shy away from.
As an International Board Certified Lactation Consultant, I have, first and foremost, an ethical obligation to provide evidence-based information to my clients to support their breastfeeding relationship. Every day, for a variety of reasons, I encounter and encourage families who need to supplement their baby’s nutrition with something other than milk directly from the mother’s breast. Today, they have many options: pump and feed their own milk, supplement with some sort of donor milk, milk-based formulas, soy-based formulas, pre-digested formulas . . . lots of options, lots of questions, lots of opportunities for parents to be confused.
The World Health Organization, in its Global Strategy for Infant and Young Child Feeding, says,
“for those few health situations where infants cannot, or should not, be breastfed, the choice of the best alternative - expressed breast milk from an infant’s own mother, breast milk from a healthy wet-nurse or a human-milk bank, or a breastmilk substitute…depends on individual circumstance.”
Since this is coming from a global authority on health, I feel pretty darn confident using this hierarchy while supporting my clients in their supplementation decisions.
Most Ideal Option - Expressed breastmilk from the infant’s own mother.
Next Most Ideal Option - Breast milk from a healthy wet-nurse…SCCRREEEEECH!!!!
When I first became aware of milk sharing, it was a “secretive” practice, one not discussed openly and one that many organizations (breastfeeding supportive and not) chose to distance themselves from. When an article appeared on TIME.com in November of 2010 about the rise of the use of social media to facilitate milk sharing, I was quick to say “What can I do to help?” because the goal seemed obvious to me: get human milk into human babies.
What I wasn’t prepared for was the strong backlash from my own professional community saying, “But what if a baby gets sick or even dies?” Quite a number of IBCLCs I know were involved in milk sharing arrangements in their own breastfeeding years and some continue to be “closeted” about their own experiences. I attended the FDA meeting in December of that year discussing the regulations in regards to donor milk and while informal sharing wasn’t formally on the agenda, it certainly was on everyone’s lips in the room. There was palpable fear that one bad outcome from milk sharing would halt all the positive momentum that breastfeeding was gaining in our culture. One expert even spat out, “These women…these women who are doing this are going to hurt or even kill their babies.” I maintain that they are simply trying to feed them the food they were designed to eat.
But, what about the RISKS, with a capital R? Wouldn’t I be putting the health and lives of the babies I serve at risk if I offer milk sharing as an option? There is nothing in life that is without risk. Is milk sharing risk-free? Absolutely not. There are also risks to breastfeeding and formula feeding. Dr. Karleen Gribble and Dr. Bernice Hausman discuss these concerns in their paper Milk Sharing and Formula Feeding: Infant Feeding Risks in Comparative Perspective. In it, they discuss the issues of contamination of milk with pathogens, chemicals, concerns with milk collection and storage hygiene. The also discuss the risks to formula use that are not present when feeding human milk. In addition, there is a section devoted to the risk of HIV from the use of shared milk. I strongly advise every breastfeeding professional as well as any mother I am working with to read this paper and discuss their concerns. Drs. Gribble and Hausman conclude that “instead of proscribing peer-to-peer milk sharing, health authorities should provide parents with guidance on how to manage and minimize the risks of sharing human milk.”
For recipients: When one of my clients is in need of milk and is considering milk sharing, I strongly encourage them to think about whether people they already know might be willing to donate. They also might explore location-based online milk sharing groups (like HM4HB), and then groups that facilitate broader-range sharing and the shipping of donor breast milk (like MilkShare). I do not condone the sale and purchase of breastmilk and I strongly encourage my clients to not consider it as an option.
No matter where the milk is coming from, I encourage my clients to thoroughly research what sorts of screening they consider essential (such as blood work from pregnancy and questionnaires about lifestyle choices such as alcohol and medication use). It is important that both parties have clear expectations about what their milk sharing arrangement looks like. At no point do I, as an IBCLC, engage with the recipient family as a “milk broker.” The family is fully responsible for finding, contacting and making arrangements with their milk donors. As an IBCLC, my role with milk recipients is only to provide information and resources.
Of note, it is always my hope that supplementation of any type can be eliminated or minimized because of an increase in a mother’s own ability to make milk. The milk sharing community is often particularly in tune with the need and desire of mothers to work hard to rebuild their milk supply. Some families get a donor and a cheerleader-in-one! Many mothers feed donor milk through the use of a supplemental feeder, which can help mothers to produce increasing amounts of their own milk by stimulating the breast while delivering the supplement. There are many stories of those who were in need of donor milk, were able to rebuild their supply and then donate milk back into the community.
For donors: I often have mothers, in their glee at how much milk their body is providing, send me an email saying they “had so much we had to dump it down the sink.” Nothing strikes panic into the heart of an IBCLC faster! If a mother tells me, as her lactation consultant, that she has more milk than she knows what to do with, I offer her information about donation. I share with her the options of contributing to a HMBANA milk bank, donating directly to another family or sharing her milk with a for-profit milk bank. (Though I have significant ethical concerns about these banks, I do share the information with my clients so that they can make the best decision for their family.)
I stress to the family that the milk they have is first and foremost for their own baby. I know that many families feel incredibly proud and thankful to be able to share of their excess. I encourage families to participate openly and honestly in all screening with their recipient family and to make sure that both parties have clear expectations about what their milk sharing arrangement looks like. At no point do I, as an IBCLC, engage with the donor family as a “milk broker.” They are fully responsible for finding, contacting and making arrangements with their milk recipients. As an IBCLC, my role with milk donors is only to provide information and resources.
An obvious question in all of this is why wouldn’t a mother in need of additional milk for her child simply obtain it from a milk bank? Then we wouldn’t be talking about risks of disease and contamination. In an ideal world, families would be able to receive ALL the milk they need from milk banks. Milk banks would be located in every community and have an unending supply of milk. I believe this can be a reality. I believe that there can be plenty of milk available to every baby that needs it. As a passionate advocate for getting human milk to human babies, Emma Kwasnica says, “milk is a free flowing resource.”
Unfortunately, in the United States, this isn’t yet the reality. As a nation, we need to drastically increase the number of milk banks and the amount of human donor milk available. The Human Milk Banking Association of North America (HMBANA) currently has 12 active banks. These banks do incredible work and, rightly so, their priority is on making sure that the MOST CRITICAL babies receive the milk that they process. For these little ones, having access to human milk can be, quite literally, a matter of life and death. Even this week, several milk banks, including those in Indiana and Utah, have issued pleas in the media for increased donations because their supplies are low. It is absolutely essential that these babies be the first to have access to processed donor milk.
Does every baby need its milk processed by a milk bank focused on the needs of vulnerable infants? For the most fragile babies, the complex processes of a milk bank (milk pooling, pasteurizing, and testing) are critical. The needs of a healthy term newborn are different. I liken it to this: If you had a dear friend who had recently received an organ transplant, you would do everything within your power to visit with them in a healthy manner by scrubbing arms and hands and wearing a mask. But, if that same friend has just gone through a “healthy” event, like birth, you would simply wash your hands. Different circumstances require different levels of caution.
Where does that leave healthy babies? In my practice, I see many mothers who, for of a variety of physical, emotional or circumstantial reasons don’t make the milk that their baby needs. At some milk banks, families of healthy babies can sometimes purchase donor milk but it is typically in limited quantities, and only available when supplies exist to meet the need of critical infants first. While the cost associated is reasonable, considering the cost of processing by the milk bank, it is often prohibitive to the families in need.
Is the only option for these families infant formula? I have every confidence that the human milk banking advocates all over the globe would affirm the belief that all babies have the right to human milk. I think that milk banking and milk sharing CURRENTLY serve very different populations of babies. Above all, my loyalties are not to milk banks or the milk sharing movement, but rather to babies and their families. There is room in the community for both methods of getting human milk to human babies.
I have been privileged to work with a number of families who were involved in milk sharing, both on the donor side and on the recipient side. I have seen milk donations have a significant impact on the health of a child. I have seen milk donations foster community that might not have happened otherwise. I have seen milk donations turn grief into hope. I have seen milk donations empower families and save babies’ lives.*
Milk sharing is not the right choice for every mother in need. Milk sharing is not the right choice for every mother who desires to donate her milk. But for many families, milk sharing facilitates health, community building, and an opportunity to reclaim the breastfeeding experience for those whose journey didn’t go as they planned.
As an International Board Certified Lactation Consultant, I have, first and foremost, an ethical obligation to provide evidence-based information to my clients to support their breastfeeding relationship. Every day, for a variety of reasons, I encounter and encourage families who need to supplement their baby’s nutrition with something other than milk directly from the mother’s breast. Today, they have many options: pump and feed their own milk, supplement with some sort of donor milk, milk-based formulas, soy-based formulas, pre-digested formulas . . . lots of options, lots of questions, lots of opportunities for parents to be confused.
I believe that parents are capable of making the choices that are best for themselves and their families.
It is my job to make sure they have all the information to do so.
“for those few health situations where infants cannot, or should not, be breastfed, the choice of the best alternative - expressed breast milk from an infant’s own mother, breast milk from a healthy wet-nurse or a human-milk bank, or a breastmilk substitute…depends on individual circumstance.”
Since this is coming from a global authority on health, I feel pretty darn confident using this hierarchy while supporting my clients in their supplementation decisions.
Most Ideal Option - Expressed breastmilk from the infant’s own mother.
Next Most Ideal Option - Breast milk from a healthy wet-nurse…SCCRREEEEECH!!!!
(do you see the virtual brakes going on???)
Wet nurse? Really? In this day and age? With HIV, hepatitis, and any number of undesirable diseases that can be passed through bodily fluids? What would wet-nursing even look like in today’s society? The first reaction of many is to simply pass off the idea as old fashioned, ancient, and outdated, not to mention dangerous. And in the United States, where I live, it is generally understood that if a mother’s own milk isn’t an option, formula is the obvious default. Why even bother?Because we, as humans, are designed to consume human milk.
In our current environment, actual wet-nursing (a woman feeding another’s baby directly at her breast) is deemed by many to be inconvenient, too intimate, and—if you will—too gross. But what about the sharing of breast milk from one mother to another? Since most mothers have access to a breast pump, it has become increasingly easy to package milk in a shareable form. And with the formation of groups such as Human Milk 4 Human Babies (HM4HB) that provide a space for families in need to connect with families who want to give, doesn’t it make sense that we would at least explore the option? Can feeding a child the milk from a mother not his own be a viable solution to our supplementation needs? Is it an option that I, as an IBCLC, am willing to share with the families in my care? I answer with a strong and firm YES.When I first became aware of milk sharing, it was a “secretive” practice, one not discussed openly and one that many organizations (breastfeeding supportive and not) chose to distance themselves from. When an article appeared on TIME.com in November of 2010 about the rise of the use of social media to facilitate milk sharing, I was quick to say “What can I do to help?” because the goal seemed obvious to me: get human milk into human babies.
What I wasn’t prepared for was the strong backlash from my own professional community saying, “But what if a baby gets sick or even dies?” Quite a number of IBCLCs I know were involved in milk sharing arrangements in their own breastfeeding years and some continue to be “closeted” about their own experiences. I attended the FDA meeting in December of that year discussing the regulations in regards to donor milk and while informal sharing wasn’t formally on the agenda, it certainly was on everyone’s lips in the room. There was palpable fear that one bad outcome from milk sharing would halt all the positive momentum that breastfeeding was gaining in our culture. One expert even spat out, “These women…these women who are doing this are going to hurt or even kill their babies.” I maintain that they are simply trying to feed them the food they were designed to eat.
But, what about the RISKS, with a capital R? Wouldn’t I be putting the health and lives of the babies I serve at risk if I offer milk sharing as an option? There is nothing in life that is without risk. Is milk sharing risk-free? Absolutely not. There are also risks to breastfeeding and formula feeding. Dr. Karleen Gribble and Dr. Bernice Hausman discuss these concerns in their paper Milk Sharing and Formula Feeding: Infant Feeding Risks in Comparative Perspective. In it, they discuss the issues of contamination of milk with pathogens, chemicals, concerns with milk collection and storage hygiene. The also discuss the risks to formula use that are not present when feeding human milk. In addition, there is a section devoted to the risk of HIV from the use of shared milk. I strongly advise every breastfeeding professional as well as any mother I am working with to read this paper and discuss their concerns. Drs. Gribble and Hausman conclude that “instead of proscribing peer-to-peer milk sharing, health authorities should provide parents with guidance on how to manage and minimize the risks of sharing human milk.”
How do IBCLCs instruct and inform clients about the risks and benefits of consuming or donating shared milk?
How do we advise our clients to mitigate those risks?
For recipients: When one of my clients is in need of milk and is considering milk sharing, I strongly encourage them to think about whether people they already know might be willing to donate. They also might explore location-based online milk sharing groups (like HM4HB), and then groups that facilitate broader-range sharing and the shipping of donor breast milk (like MilkShare). I do not condone the sale and purchase of breastmilk and I strongly encourage my clients to not consider it as an option.
No matter where the milk is coming from, I encourage my clients to thoroughly research what sorts of screening they consider essential (such as blood work from pregnancy and questionnaires about lifestyle choices such as alcohol and medication use). It is important that both parties have clear expectations about what their milk sharing arrangement looks like. At no point do I, as an IBCLC, engage with the recipient family as a “milk broker.” The family is fully responsible for finding, contacting and making arrangements with their milk donors. As an IBCLC, my role with milk recipients is only to provide information and resources.
Of note, it is always my hope that supplementation of any type can be eliminated or minimized because of an increase in a mother’s own ability to make milk. The milk sharing community is often particularly in tune with the need and desire of mothers to work hard to rebuild their milk supply. Some families get a donor and a cheerleader-in-one! Many mothers feed donor milk through the use of a supplemental feeder, which can help mothers to produce increasing amounts of their own milk by stimulating the breast while delivering the supplement. There are many stories of those who were in need of donor milk, were able to rebuild their supply and then donate milk back into the community.
 |
| Photo via World Milksharing Week on Flickr |
I stress to the family that the milk they have is first and foremost for their own baby. I know that many families feel incredibly proud and thankful to be able to share of their excess. I encourage families to participate openly and honestly in all screening with their recipient family and to make sure that both parties have clear expectations about what their milk sharing arrangement looks like. At no point do I, as an IBCLC, engage with the donor family as a “milk broker.” They are fully responsible for finding, contacting and making arrangements with their milk recipients. As an IBCLC, my role with milk donors is only to provide information and resources.
An obvious question in all of this is why wouldn’t a mother in need of additional milk for her child simply obtain it from a milk bank? Then we wouldn’t be talking about risks of disease and contamination. In an ideal world, families would be able to receive ALL the milk they need from milk banks. Milk banks would be located in every community and have an unending supply of milk. I believe this can be a reality. I believe that there can be plenty of milk available to every baby that needs it. As a passionate advocate for getting human milk to human babies, Emma Kwasnica says, “milk is a free flowing resource.”
Unfortunately, in the United States, this isn’t yet the reality. As a nation, we need to drastically increase the number of milk banks and the amount of human donor milk available. The Human Milk Banking Association of North America (HMBANA) currently has 12 active banks. These banks do incredible work and, rightly so, their priority is on making sure that the MOST CRITICAL babies receive the milk that they process. For these little ones, having access to human milk can be, quite literally, a matter of life and death. Even this week, several milk banks, including those in Indiana and Utah, have issued pleas in the media for increased donations because their supplies are low. It is absolutely essential that these babies be the first to have access to processed donor milk.
Does every baby need its milk processed by a milk bank focused on the needs of vulnerable infants? For the most fragile babies, the complex processes of a milk bank (milk pooling, pasteurizing, and testing) are critical. The needs of a healthy term newborn are different. I liken it to this: If you had a dear friend who had recently received an organ transplant, you would do everything within your power to visit with them in a healthy manner by scrubbing arms and hands and wearing a mask. But, if that same friend has just gone through a “healthy” event, like birth, you would simply wash your hands. Different circumstances require different levels of caution.
Where does that leave healthy babies? In my practice, I see many mothers who, for of a variety of physical, emotional or circumstantial reasons don’t make the milk that their baby needs. At some milk banks, families of healthy babies can sometimes purchase donor milk but it is typically in limited quantities, and only available when supplies exist to meet the need of critical infants first. While the cost associated is reasonable, considering the cost of processing by the milk bank, it is often prohibitive to the families in need.
Is the only option for these families infant formula? I have every confidence that the human milk banking advocates all over the globe would affirm the belief that all babies have the right to human milk. I think that milk banking and milk sharing CURRENTLY serve very different populations of babies. Above all, my loyalties are not to milk banks or the milk sharing movement, but rather to babies and their families. There is room in the community for both methods of getting human milk to human babies.
I have been privileged to work with a number of families who were involved in milk sharing, both on the donor side and on the recipient side. I have seen milk donations have a significant impact on the health of a child. I have seen milk donations foster community that might not have happened otherwise. I have seen milk donations turn grief into hope. I have seen milk donations empower families and save babies’ lives.*
Milk sharing is not the right choice for every mother in need. Milk sharing is not the right choice for every mother who desires to donate her milk. But for many families, milk sharing facilitates health, community building, and an opportunity to reclaim the breastfeeding experience for those whose journey didn’t go as they planned.
Again, I affirm that parents are capable of making the choice that is best for their families.
It is my job to make sure they have all of the information to do so.
*A nod to Ursuline Singleton for her statement at the 2012 ILCA Conference that “IBCLCs empower mothers and save babies’ lives.” Thank you, Ms. Singleton, for so clearly helping to define what is essential to my profession.10 Sept 2012
What is World Milksharing Week?
World Milksharing Week 2012 is nearly upon us! I am excited for all the learning and celebrating taking place this year. To kick off WMW 2012's blog carnival, here is a wonderfully informative post by Dinnae Galloway, blogger at Complete Wellness Concept. She answers questions like, "What is World Milksharing Week anyway? And why do we need it?" As a Human Milk 4 Human Babies and WMW 2012 volunteer, Dinnae gives us an insider's perspective on all the buzz:
If you didn’t know, I’m a volunteer admin for my local Human Milk 4 Human Babies chapter (or HM4HB for short). I help, along with a handful of other dedicated, awesome chicks, to run the facebook page where peer-to-peer milksharing connections in BC happen. What is HM4HB you ask? Well, from the HM4HB website:
WMW stands for World Milksharing Week. This year will mark the 2nd Annual World Milksharing Week, and oh are we ever excited!
Why was WMW created? Again, this time from the WMW website:
Would you like to see how you can help? Do you have a milksharing story to share? As a donor? As a recipient? I’d love to hear about it, and so would the rest of the WMW 2012 Committee. You can submit your stories here, or feel free to comment here!
If you didn’t know, I’m a volunteer admin for my local Human Milk 4 Human Babies chapter (or HM4HB for short). I help, along with a handful of other dedicated, awesome chicks, to run the facebook page where peer-to-peer milksharing connections in BC happen. What is HM4HB you ask? Well, from the HM4HB website:
And what is WMW 2012, I’m SURE you’re asking as a follow up, no? ;)HM4HB is a global milksharing network, a virtual village, comprised of thousands of people from over fifty countries. We are mothers, fathers, adoptive families, grandparents, childbirth and breastfeeding professionals, volunteers, supporters, donors, and recipients that have come together to support the simple idea that all babies and children have the right to receive human milk. We use social media as a platform for local families to make real-life connections and come together as sustainable milksharing communities where women graciously share their breastmilk. HM4HB is built on the principle of informed choice: we trust, honour, and value the autonomy of families and we assert they are capable of weighing the benefits and risks of milksharing in order to make choices that are best for them. We hold the space for them and protect their right to do what is normal, healthy, and ecological.
| The WMW Logo |
Why was WMW created? Again, this time from the WMW website:
So, not only do I volunteer with HM4HB ~ BC, I also am part of the WMW 2012 Committee. I was part of it last year, and excited to be part of it again this year. What do *I* do, as a volunteer? Well, it’s kinda fun. I blog, I post, I pin, I tweet. I respond to emails, I post pics to the WMW 2012 Gallery, and stories to the WMW site. And in the last week of September 2012, I will be co-hosting a World Milksharing Week Event again, most likely a potluck picnic like last year. :) Fun times, with the families that benefit from, support and encourage peer-to-peer milksharing!World Milksharing Week is held annually during the last week of September. Our goalis to celebrate milksharing and to promote human milk as the biologically normal nourishment for babies and children.World Milksharing Week was born within Human Milk 4 Human Babies Global Network. The network launched the first ever World Milksharing Week, which took place from September 24-30, 2011, all around the planet. The logo was designed by HM4HB community page administrator, Dani Arnold-McKenny.We hope that by raising awareness about milksharing, families will never again feel forced into feeding breastmilk substitutes -an act which is not without risk to the health of the child. The incredible sense of community that is created among donor and recipient families who partake in milksharing is to be celebrated.
Would you like to see how you can help? Do you have a milksharing story to share? As a donor? As a recipient? I’d love to hear about it, and so would the rest of the WMW 2012 Committee. You can submit your stories here, or feel free to comment here!
14 Dec 2011
A Gay Man's Guide to Breastfeeding: If I Can Do It, So Can You!
Note: This is about as far from medical advice as you can get.
Step One: Plan a home birth. If this is not possible for you, choose a nearby field preferably with tall, sweet-smelling grass. If you are more woodsy-minded, a small stand of trees will also do nicely.
Step Two: Gawk at people who are breastfeeding successfully. DO NOT politely avert your eyes at the sight of a bare human nipple, but instead, stare at it. Observe how the baby latches on.
Step Three: Birth on your own time, with privacy. Ask someone who has breastfed a child for at least one year to be on-call and ready to help you within an hour of the birth. DO call this person if you experience any difficulty latching your baby, or even if you are just not quite sure!
Step Four: Immediately after the birth, DO stay with your baby. DO NOT weigh or bathe your baby. BREASTFEED your baby.
Step Five: Breastfeed.
Step Six: Breastfeed.
Step Seven: Breastfeed.
Step Eight: Breastfeed.
Step Nine: Breastfeed.
Step Ten: If after all this breastfeeding, you still don't have enough milk, get some donated breast milk from a friend or through Human Milk 4 Human Babies.
Step Eleven: Keep breastfeeding. Use a supplemental nursing system if you need to.
Step One: Plan a home birth. If this is not possible for you, choose a nearby field preferably with tall, sweet-smelling grass. If you are more woodsy-minded, a small stand of trees will also do nicely.
Step Two: Gawk at people who are breastfeeding successfully. DO NOT politely avert your eyes at the sight of a bare human nipple, but instead, stare at it. Observe how the baby latches on.
Step Three: Birth on your own time, with privacy. Ask someone who has breastfed a child for at least one year to be on-call and ready to help you within an hour of the birth. DO call this person if you experience any difficulty latching your baby, or even if you are just not quite sure!
Step Four: Immediately after the birth, DO stay with your baby. DO NOT weigh or bathe your baby. BREASTFEED your baby.
Step Five: Breastfeed.
Step Six: Breastfeed.
Step Seven: Breastfeed.
Step Eight: Breastfeed.
Step Nine: Breastfeed.
Step Ten: If after all this breastfeeding, you still don't have enough milk, get some donated breast milk from a friend or through Human Milk 4 Human Babies.
Step Eleven: Keep breastfeeding. Use a supplemental nursing system if you need to.
Subscribe to:
Posts (Atom)