This
information is free for personal use. Any trans folk are welcome to
print it out and give a copy to their health care provider! However, if
you wish to publish any part of it or quote this material in a
presentation you must obtain formal permission. Thanks!
I'm not a health care professional and this blog entry does not constitute or replace medical advice. Please consult your doctor if you need medical advice.
**** This blog post has been updated and now comes in three parts: 1) general information 2) assisting trans men 3) assisting trans women
Transgender/transsexual/genderfluid
Tip Sheet - General Information
Prepared
by Trevor MacDonald
This tip
sheet provides some key details you should be aware of when offering
reproductive/lactation support to transgender, transsexual, or genderfluid individuals.
Keep in mind that in most ways, medically and otherwise, trans people are just
like everyone else. There is a list of key terms and their definitions at the
end of this sheet.
Gender vs. Sex
Our
reproductive organs and sexual anatomy define our physical sex - male, female, or intersex. Gender, however, is a person's inner awareness of their femininity/masculinity. Gender expression has to
do with how an individual presents their gender to others within a given
cultural context. For example, within western culture the colour pink has gone
from being a traditional boys' colour to one for girls in only a few
generations.
In most
cases, a person’s biological sex conforms to
their gender and gender expression. The term for such people is cisgender.
Transgender, transsexual, and genderfluid people have a gender identity or
gender expression that does not match what their particular society expects of
them according to their anatomy. Some trans people choose to use medical
therapies such as hormone treatments and/or surgeries to alter their bodies.
Others do not want or are unable to obtain such interventions, but may express
their gender in other ways such as choices of clothing or makeup.
Gender Identity vs Sexual Orientation
A
person's gender identity has to do with how they self-identify. Their sexual
orientation refers to what kind of person they are sexually attracted to. A
person can be trans and gay, or trans and straight, or trans and bisexual, etc.
Asking Questions
It may be
essential to ask questions regarding an individual's gender identity or history
of medical transition in order to provide adequate care. However, only ask
those questions that are relevant. Do not
ask questions solely out of curiosity.
Language
Always
use the pronouns that refer to an individual's expressed gender, not their
assigned birth sex. For example, a male-to-female transsexual woman is 'she'.
If you are unsure of which pronouns a particular individual may prefer, simply
ask in a respectful manner. If you make a mistake, apologize promptly and move
on. Some people prefer gender-neutral pronouns, such as 'them' and 'they' or
'ze' and 'zir'.
The
following terms are derogatory. Do not
use: tranny, he-she, she-male, gender-bender, or transvestite.
Do not refer to someone 'masquerading',
'pretending', 'disguising', etc. in their gender.
Use
transgender as an adjective, not a noun or verb.
He is a transgender person, not "He is a
transgender." (similar to how it is best to
say "He is a black person", rather than "He is a
black")
A person is transgender, not
transgendered. It is never necessary
to add the suffix 'ed' to transgender.
Common terms
*Note
that these definitions explain how the following terms are generally
understood. However, individuals within the trans community may define them
differently or may self-identify outside of these labels.
cisgender: someone whose gender identity matches their assigned
birth sex (they are not transgender)
FtM:
female-to-male trans person
MtF:
male-to-female trans person
gender binary: The notion that there are two genders, male and female.
Many trans people understand gender as a spectrum.
gender expression: a person's outward presentation of their gender through
physical traits, clothing, makeup, etc.
genderfluid/genderqueer: someone who identifies between or beyond the extremes of
female and male on the gender spectrum, or who identifies as both female and
male at once or as some combination of genders.
gender identity: a person's inner sense of their gender.
intersex:
a condition in which an individual is born with reproductive and/or sexual
anatomy that does not fit the usual male or female definition.
trans:
an umbrella term meant to include transgender, transsexual and genderfluid
people
transgender: a person whose gender identity or expression does not
match the typical societal expectations of their birth-assigned gender.
Transgender people may or may not wish to modify their bodies to varying
degrees by taking hormones or having surgery.
transition: a change in one's public
gender identity (one's inner gender identity may have been the same since
birth).
transsexual: a person whose gender identity does not match their sex
as it was assigned at birth. Transsexual people usually wish to modify their
bodies in order to alleviate this incongruence.
Tip
sheet for assisting trans men
Trans men
are individuals who were born with anatomy typical of females but identify on
the masculine side of the gender spectrum. Some choose to give birth and/or
nurse their babies, and may require lactation support.
Language
Although
both men and women have breast tissue, the word 'breast' is most often
associated with women. Trans men may be more comfortable referring to their
'chest' and 'chestfeeding' or 'nursing' their infants, rather than
'breastfeeding'. Trans men may refer to themselves as 'dad', 'papa', or another
term, rather than 'mom'. Don't make
assumptions. Remember that if you are unsure, it is best to ask about which
names and pronouns an individual prefers to be used. If you make a mistake,
apologize promptly and move on.
Testosterone Use
Many, but
not all, trans men choose to take testosterone. Testosterone normally causes
the cessation of menstruation and ovulation, and brings about male secondary
sex characteristics such as deepening of the voice, growth of facial hair, and
male pattern baldness.
When a
trans man stops taking testosterone, his cycles are likely to return after
several weeks or months, depending on how long he took the medication and his
own physical particularities. However, most of his male secondary sex
characteristics will remain. For example, once testosterone has stimulated the
growth of hair follicles in a person's face, those follicles will stay there
and hair will keep growing unless extensive electrolysis treatments are
undertaken (a common element of male-to-female individuals' transitions).
Although
very rare, some trans men have been known to become pregnant accidentally while
taking testosterone. Testosterone is highly toxic to the fetus and should never
be used during pregnancy. However, because the body metabolizes and clears
testosterone rapidly, it is considered safe to conceive within a few months of
discontinuing most forms of testosterone therapy.
Testosterone
use during the period of lactation would likely interfere with the hormones
required to produce milk and achieve let-down.
Top Surgery
Some
trans men choose to have male chest-contouring surgery, also known as 'top
surgery'. This is different from a mastectomy (a cancer treatment), or a breast
reduction, which is performed to make a smaller but still female chest. The
goal of top surgery is to create a male-appearing chest. In order to do this
some, but not all, of the client's
mammary tissue is removed. Complete removal of the mammary tissue would result
in a sunken chest shape.
The
preferred surgical technique for top surgery is variable, depending on factors
such as volume of tissue and skin elasticity of the client. The 'double
incision' technique usually involves nipple grafts, and is not ideal for
maintaining nipple sensation nor preserving milk ducts. The 'peri-areolar'
approach, with incisions that go around the outer borders of the areolae,
leaves the nipple stalks intact and likely has better results in terms of
future breastfeeding and milk production.
Binding
A trans man who has not had top surgery may choose to bind his
chest in order to flatten it, thereby managing his gender dysphoria. Many years
of binding may adversely affect the glandular tissue. Binding during the
immediate postpartum period will increase the risk of blocked ducts and
mastitis and may damage the milk supply. However, some individuals have had
success with occasional, careful binding once the milk supply is well
established and regulated. Anyone who practices binding during the lactation
period should be advised of the risks of doing so, and should monitor the
health of their chest closely.
Chestfeeding Goals
Some
trans men who give birth do not want to chestfeed at all, in some cases for
reasons to do with mental health. Others do, and opt to postpone desired top
surgery so that they will be able to produce a full milk supply. Others who
have had top surgery may still wish to develop a nursing relationship and may
do so using an at-chest (at-breast) supplementer.
Gender Dysphoria and Chestfeeding
Gender
dysphoria occurs when an individual feels discomfort due to parts of their body
that do not match their gender identity. Growth (or re-growth after top
surgery) of chest tissue during pregnancy may bring up extreme feelings of
gender dysphoria in some individuals, possibly causing anxiety or even
depression. Chestfeeding can do the same. For this reason, deciding to
chestfeed is a very personal choice.
Supporting the Decision NOT to Nurse
Support an individual who has chosen not to chestfeed by sharing
how he can quickly reduce his milk supply after the birth. Explain the supply
and demand system that governs lactation. Encourage the client to remove only
as much milk as necessary to feel relatively comfortable, since removing more
milk will cause the body to increase production. Cold compresses and cold
cabbage leaves may help reduce pain and swelling. The parent should NOT bind at
this time due to the increased risk of pain, blocked ducts, and mastitis. Several
herbs such as sage, peppermint, and parsley are said to decrease milk supply.
Discuss the many other ways of bonding with baby, such as bed-sharing,
babywearing, and loving, attentive feeding. You may wish to let the client know
about the possibility of obtaining human milk through milk sharing sites such
as Human Milk 4 Human Babies or Eats on Feets.
Supporting the Decision TO Nurse
Be
respectful when providing ‘hand-on’ care. As in most health care situations, ask permission
before touching an individual's body, explaining what you are planning to do
and why. If an individual is not comfortable being touched, find other ways to
help, such as demonstrating on yourself.
Watch for
signs of postpartum depression. Trans individuals may be particularly at risk
due to struggling with gender dysphoria in addition to the usual challenges of
giving birth and caring for a newborn.
When
assisting those who wish to chestfeed after a previous top surgery, it is
essential to remember that nursing a baby is not only about the milk. An
individual who has had surgery may produce a surprising amount of milk, or only
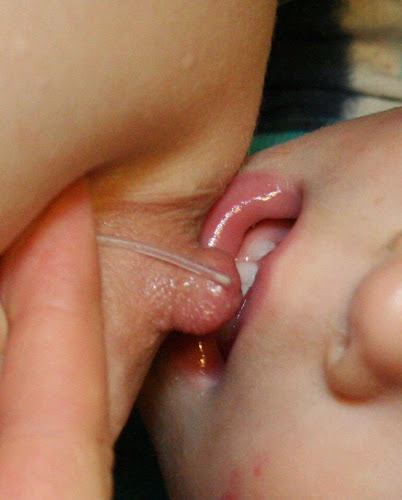
drops, or nothing at all. Any amount of milk is valuable. By using a
supplementer, the parent and baby can gain the benefit of bonding through a
nursing relationship even in the absence of milk production. In addition, the action of nursing helps promote the
normal development of the jaws and teeth in the infant.
Latching
may be challenging for the parent who has had previous top surgery due to a
relative lack of pliable tissue and skin. The parent may need to learn how to
vigorously mould the chest tissue (make a 'sandwich'). When providing
assistance, be creative and expect to try many different grasps from varying
angles in order to find what works.
A
reclining position may unfortunately cause the chest tissue to become even more
taut and difficult to latch to. In this case, football hold or cross cradle may
be easier.
Support Meetings
Encourage
the trans breastfeeding parent to attend group meetings and ensure that a safe
and positive environment is provided. We know that peer support is an important
predictor of a parent's success achieving their personal breastfeeding goals.
Trans parents may already feel isolated, especially if they do not know other
LGBT families. Group meetings can be tremendously beneficial.
Those
facilitating the meeting should know the location of a men's washroom or gender
neutral washroom near the meeting room. They should use gender-neutral language
such as "breastfeeding parent" instead of "mother" when
addressing the group.
Other Support and Resources
The
community of trans individuals interested in birth and various infant feeding
methods is growing fast. At this time, the only online support group is the
Facebook-based Birthing and Breastfeeding Transmen and Allies, with over 500members worldwide. The group includes many interested and supportive lactation
consultants and LLL Leaders.
Toronto's
LGBT Parenting Network runs a weekend course once every few years for
transmasculine individuals considering pregnancy.
Diana West's book, Defining Your Own Success: Breastfeeding After Reduction Surgery, contains information relevant to trans men who have had top surgery. Also see her web site, bfar.org.
Tip
sheet for assisting trans women
Trans
women are individuals who were born with anatomy typical of males but identify
on the feminine side of the gender spectrum. Some trans women may wish to
breastfeed their children via induced lactation and/or using a supplementer.
Inducing Lactation
Trans
women may induce lactation by following the Newman-Goldfarb protocol. A
physician would need to prescribe the appropriate medications. Birth control
pills should be started about six months before the baby is expected or as soon
as possible. Domperidone is also suggested in the protocol. 6-8 weeks before
the birth, the birth control pills should be stopped, and the woman should
begin pumping frequently to stimulate glandular tissue and to remove milk. The
domperidone is normally continued for the duration of the lactation period.
A trans
woman should discuss with a physician, such as a reproductive endocrinologist,
what kind of hormone treatment is best to take during lactation. Unfortunately,
there has been little to no research done in this area. Some trans women have
successfully taken a decreased dose of their usual estrogen while lactating.
Any medications, such as anti-androgens or estrogens, should be carefully
considered for safety during lactation on an individual basis.
Expectations
Some
trans women have induced lactation with impressive results, providing nearly a
full supply to their babies. The amount of milk that is produced will depend
somewhat on how many years the women used hormones prior to inducing lactation,
and how fully her glandular tissue developed during that time. If the woman had
implant surgery, she may encounter some difficulty with severed ducts, damaged
nerves, compressed glandular tissue, and/or scarring.
As is the
case with chestfeeding trans men, the amount of milk that is produced is not as
important as the nursing relationship itself. An at-breast supplementer may be
used to support a nursing relationship.
Support Meetings
Encourage
the trans breastfeeding parent to attend group meetings and ensure a safe and
positive environment is provided. We know that peer support is an important
predictor of a parent's success achieving their personal breastfeeding goals.
Trans parents may already feel isolated, especially if they do not know other
LGBT families. Group meetings can be tremendously beneficial.
Resources and Further Information
"Trans
Women and Breastfeeding: A Personal Interview" by Trevor MacDonald,
available at http://www.milkjunkies.net/2013/05/trans-women-and-breastfeeding-personal.html.
"Trans
Women and Breastfeeding: The Health Care Provider" by Trevor MacDonald,
available at http://www.milkjunkies.net/2013/07/trans-women-and-breastfeeding-health.html
Facebook-based
Birthing and Breastfeeding Transmen and Allies group welcomes trans women
interested in nursing their infants.
Diana
West's book, Defining Your Own Success: Breastfeeding After Reduction
Surgery, contains information relevant to trans women who have had breast
surgery. Also see her web site, bfar.org.