26 Jun 2018
Breastfeeding/Chestfeeding and Gradual Weaning: A Snapshot in Time
1 Jan 2014
Resolution: Tackle Inner Transphobia
2 Jul 2013
Trans Women and Breastfeeding: The Health Care Provider
For the previous post in this series, I interviewed a trans woman who is enjoying a wonderful breastfeeding relationship with her baby. It was amazing and so valuable to get a firsthand perspective from someone who has "been there, done that."
Today's post focuses on the health care provider's perspective. Over the last few weeks, I've chatted with Mary Lynne Biener, IBCLC, and Jack Newman, MD, at the International Breastfeeding Centre in Toronto, as well as Diana West, IBCLC, a co-author of The Womanly Art of Breastfeeding and other titles. Mary Lynne and Jack have some limited experience working with trans women interested in breastfeeding.
You'll notice that several times my questions were answered with some variation of, "We just don't know!" I think it's important to point that out. We need research in this area. I'll try here to share what is known and highlight what is not.
Trevor MacDonald: Generally speaking, what do you think health care providers need to know in order to assist trans women interested in breastfeeding?
MaryLynne Biener, IBCLC: I think it's important to have at least a basic working knowledge of the various aspects of transition (medical, social, and emotional). While it's great to ask questions about an individual's experience (where appropriate) and breastfeeding goals, it's not ok to expect a "trans 101" lesson from a client/patient. Don't try to learn off of someone's back. As practitioners, we must examine our own assumptions and do our own work around educating ourselves. Also, there are aspects of transition that are not relevant to lactation - it's important to stick to what is within one's scope of practice. Be knowledgable about terminology and if you're not sure, ask about pronouns and language relevant to an individual.
I think it's also important to inform the client about what induced lactation can look like - that she may or may not produce all the milk her baby needs. At the same time, help her learn that there's way more to breastfeeding than just the milk. How can we support her in 1) maximizing what she produces and 2) supplementing (if needed) in a way that is compatible with breastfeeding (including accessing donated human milk)?
Realize that a lot of this is unknown territory and that this aspect of lactation support is evolving. Be open to new information, and be open to feedback.
Trevor: Which medications should trans women take to induce lactation? Is this recommendation the same as the protocol for inducing lactation in adoptive cisgender mothers?
Mary Lynne: So far we have done the same protocol. In a nutshell, and depending on the number of months before the estimated "due" date, we suggest a combination of the birth control pill (to mimic pregnancy, one should take the active pills only and no placebos) and domperidone. One would stop the birth control pill about 6-8 weeks before the baby is expected and start the pumping protocol but stay on the domperidone. Pumping is key, as it is stimulation of the glandular tissue and milk removal that promote milk production. Especially if there is not another breastfeeding or chestfeeding partner with a full supply, it makes sense to have a head start in promoting milk production via pumping and domperidone. Sometimes we also suggest starting herbs such as fenugreek, blessed thistle and, more recently, moringa leaf.
Is this enough? We don't know. I'm guessing that it could become challenging once the birth control pill is stopped…does the woman continue to require hormones (for a variety of reasons) and would this have an impact on milk supply? Unfortunately, I don't have an answer to that.
Trevor: In what ways do you think factors such as previous breast implant surgery, number of years on hormone therapy, or the age at which a woman began her transition would affect her milk supply?
Diana West, IBCLC: Any woman's ability to breastfeed depends on her lactation infrastructure, which includes intact nerves, ducts, and well-developed glandular tissue. Assuming the surgery was done in such a way that the nerves are intact and she has normal nipple sensation, the next question becomes where the implants are. Those below the muscle tend to result in the best milk production, probably because they don't compress the glandular tissue directly.
Severed ducts is a more complex issue. In cis-women, each menstrual cycle prompts glandular growth so that by her early twenties, there is usually a bare-bones glandular infrastructure. Unless they began hormonal therapy during adolescence, trans women may not have this head start. But it's possible that this could actually work in their favor. Fewer ducts at the time of the surgery may mean fewer ducts available to cut. If most of the glandular tissue growth is prompted after the surgery, most of the ducts that develop will be intact.
The amount of glandular tissue that develops will not be affected by implants, but if she induces lactation with a hormonal therapy and the implants are above the muscle, she may find that her breasts become painful as the glandular tissue develops.
The most important thing that a trans mother who has had implant surgery should take to heart is that nursing a baby is not about the amount of milk she makes, but rather the amount of love that she pours into her baby while she nurses him.
MaryLynne: As with cisgender women, there may be an issue regarding scarring (especially if the scars are periareolar) - this has to do with the pliability of the nipples and areolae and the ability of the baby to latch deeply. I'm guessing that the more years of hormone therapy, the better in terms of breast tissue development (and the older the surgery is, the greater chance of recanalization of nerves and ducts). Age at transition may be a factor simply in terms of the potential number of years on hormonal therapy.
Trevor: Do trans women typically face any special challenges in latching their babies?
MaryLynne: I'm not sure. It would depend on an individual woman's anatomy, history of surgeries, what interventions happened during and following the birth (issues on the baby's end), how much support she has, etc.
Trevor: Could there be particular troubles due to having less fully developed glandular tissue? Do folks with insufficient glandular tissue (IGT) have more latching issues than others?
MaryLynne: I don't think that IGT necessarily interferes with latching per se. What can be problematic are common interventions that interfere with breastfeeding. For example, if someone has IGT and isn't producing enough milk (even colostrum), one of the more common interventions is to supplement with a bottle, which we know can cause significant latching issues.
Trevor: In my last post, the trans woman I interviewed about her experience with induced lactation told me that when she produced her first drops of milk they were waxy in consistency. They became thinner until like normal milk. Is this a common experience with induced lactation?
MaryLynne: Sounds like colostrum to me (which can be quite thick and waxy). And yes, I have seen that with induced lactation in cisgender women as well.
Trevor: Are there any trans-related medications that women should avoid while breastfeeding? eg. I've been told that some anti-androgens may not safe be to take while breastfeeding.
MaryLynne: I think we would have to judge each medication individually as we do with any medications (for example, antidepressants are compatible with breastfeeding, however some are more compatible than others). There are few medications that are completely incompatible with breastfeeding, so I think we would treat anti-androgens like any other medication: we would consider the half-life, degree to which it is protein-bound, its solubility, its molecular size, etc, and then help the client understand the risks and benefits involved.
Dr. Jack Newman: We can worry about anti-androgen medications if the mother produces significant amounts of milk. But in theory, they should help with production.
Trevor: How successful have female trans clients you've known or communicated with been in their breastfeeding journeys?
MaryLynne: I have only worked with one woman and it was a prenatal visit. I haven't heard any feedback. Yet :)
Jack: Our experience is limited. But the idea is feeding the baby at the breast, not necessarily making lots of milk. The latter would be nice, but most women inducing lactation don’t produce all the milk the baby needs.
Health care providers need to know that this is a worthwhile thing to do. The rest will follow. They can refer. They can learn.
31 Oct 2012
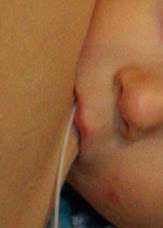
Using an At-Chest Supplementer
 |
| Making an at-chest supplementer is easy and cheap. |
Using an at-chest (at-breast) supplementer is a great way to feed your baby if you are unable to produce all of the milk he or she requires. This method is completely supportive of the nursing relationship, and does not involve your baby latching on to any artificial nipples, such as bottle nipples. As wonderful as it is, this kind of supplementer can be brutally hard to use at first. I've been using one for over eighteen months, so I'll share some tips!
First, let me explain what it is. All the different versions consist of a container to hold the supplement and a long, narrow tube. One end of the tube goes into the supplement, and the other end is placed right by your nipple. Your baby latches onto both the tube and your nipple simultaneously, drawing supplement from the container and getting all the milk that you are producing, too.
What's great about it? Using an at-chest supplementer allows you to do all feedings at your own chest. This is amazing for your nursing relationship and all the bonding that comes with it. It's also important for promoting normal jaw development in the infant - the physical action of chestfeeding develops a baby's muscles differently than bottlefeeding does. Using the supplementer helps you produce more milk, too, because even at times when your baby is only receiving supplement and you are not producing any milk, your chest tissue is being stimulated to make more. For those who produce little to zero milk, using the supplementer makes it possible to still have a nursing relationship.
How do I get one? You can buy a commercial supplementer, or you can easily and cheaply make your own. I prefer the homemade kind, so that's what I'll describe first. You can use any baby bottle to hold your supplement. Get gavage tubes from a pharmacy, or in bulk from a medical supply store. The kind to look for is 5 French (that's the diameter), 36 inches in length. You might want a tube with a bigger diameter if your baby has a weak suck, a complication of some conditions such as cleft palate or prematurity. Using a shorter tube is super irritating because it forces you to hold the supplement container so close to your baby's mouth (who has enough hands to do all that?!). Cut off the extra plastic bits, if there are any, on one end of the tube. The other end will be closed and rounded and will have two or three holes just before the tip - I cut off this part too because otherwise the supplement doesn't seem to come out easily. Some don't do this because they believe that cutting this end makes the tube sharp (we never experienced a problem with this). Thread one end of the tube through the bottle nipple (expand the opening of the nipple with a knife if required) so that it is sitting in the supplement. To clean the tube after use, just suck some hot water through it. Do not boil this kind of tube - it is not made from materials designed to withstand such a hot temperature.
The main difference between the homemade and commercial systems is cost. The Lact-Aid is $48.75 or $62.50, depending on whether you get the deluxe or standard model. The Supplemental Nursing System (SNS), made by Medela, was $42.99 on Amazon when I checked at the time of writing. It should be noted that Medela is a company that violates the World Health Organization's code on the marketing of bottles and artificial nipples. Unfortunately, its product name, SNS, is often incorrectly used as a generic name for a supplementer. You can make your own supplementer for the cost of any baby bottle and nipple and a $5.00 gavage tube. If you use this system in the long-term, you will end up spending a fair bit on tubes. They can be bought in bulk for about $1.00 a piece, and most people replace them once per week (or when they get too stiff to use) - so, you could spend $52 on tubes if you use the homemade supplementer for one year. I've been told by several people who used an SNS or Lact-Aid for over a year that both systems hold up very well to wear and tear and rarely need replacement parts.
With both the SNS and the Lact-Aid, the supplement container hangs around your neck. I like my homemade version because I can put the container down beside me on a table or hold it between my knees - I hated the idea of something relatively heavy dangling from my neck. I also like being able to have a decent amount of supplement on hand. The containers of the SNS (re-usable) and Lact-Aid (disposable bags) are smaller than most baby bottles. My number one reason for using my homemade version is that it is simpler - it has only three parts (bottle, nipple, and tube).
 |
| Moulding the chest tissue and positioning the tube |
There's a lot to have to juggle between latching your newborn and placing a tube. This is how I do it: I get my baby in position and latch him first without the tube (otherwise he gets too antsy waiting for me to have everything ready). Then I take the end of the tube and get it near the end of my nipple. I briefly un-latch my baby. I use my thumb and middle finger to mould my chest tissue into a shape that my baby can latch to, and use my index finger to position the tube so that the end of it is in line with the tip of my nipple. The tube comes from above my nipple so that it points to the roof of my baby's mouth when he latches. I slip my index finger out of the way just as he is latching on and then I hold the tube in place for an extra second or two until the supplement is flowing up the tube. Some people tape the tube to their chest, but this didn't work for me. The tube would always flip in the wrong direction when I tried to mould my chest tissue for my baby to latch.
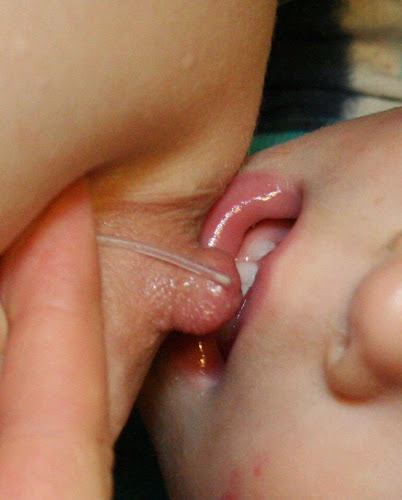 |
| About to latch |
Have you used a supplementer? Do you have any additional tips to share that we should know about?
24 Aug 2012
Why I Can Support Breastfeeding Women
In the past few days, some have mentioned they are concerned that women would not feel comfortable seeking breastfeeding advice from a man, or even attending a meeting when a man is present. Fortunately, I have not personally encountered anything like this at my local La Leche League meetings. I have attended a number of meetings together with brand-new, first-time moms, and these moms have shared openly at meetings and returned to meetings. I believe that a man who breastfeeds is perceived very differently from a man who does not.
What those of us who attend meetings have in common is that we want to breastfeed our kids. Early in my pregnancy, I did tons of reading about breastfeeding, and one thing that came up over and over again was this: a huge predictor of whether or not you will succeed in breastfeeding as long as you want to is if you have good community, peer support. I used to read that and say to myself, "Except for me. I don't count." When I did in fact get to go to an LLL meeting before my baby was born, I was incredibly grateful. I walked into the meeting shaking with nerves. I could barely speak when it was my turn to introduce myself and I explained my unique situation. I was terrified of what people would think of me and how they would react. I looked up at a certain point and realized that the women there were smiling at me and nodding their heads as they listened to me.
When we talk about experiences of oppression and fear, I feel that I have those in common with breastfeeding women. I was yelled at by a WOMAN for breastfeeding my baby in public - she said I was ruining my child. I spoke calmly to her at the time but cried for quite a while after it was over, feeling terrible. I get stared at when I breastfeed. There are some places where I don't breastfeed because it simply isn't safe. As a transgender guy nursing in public, I am not exactly in a position of power over others. I believe that any woman who learns in 30 seconds or so that I breastfeed my baby (and of course, having breastfed is a requirement for being a volunteer leader) will know that I have been through the same grief as any other breastfeeding person.
Men who have never breastfed have not experienced firsthand what breastfeeding parents have. Similarly, if a bunch of judgemental female OB's showed up at an LLL meeting, the breastfeeding women would probably not feel comfortable. In our chapter, when a non-breastfeeding medical professional wants to attend a meeting, she must gain special permission and she is asked not to contribute to discussion. I believe this whole issue is not simply about sex or gender, but about the common experience of breastfeeding, which in our society seems unfortunately to have a lot to do with oppression.
I try to keep my attitude in life, as well as my writing, positive. On the whole, our family has received FAR more support and well-wishes than any other kind of comment (I'm talking about personal emails, Facebook messages, and blog comments - I never read comments on news articles). However, I don't think that anyone breastfeeding in public in North America today can do so without at least a hint of fear or doubt, and I am certainly no exception. This is why we need La Leche League - a safe space to share accurate, science-based information about breastfeeding without judgement.
10 Jun 2012
Petition to Ease Restrictions on Breast Milk in Carry-On Baggage
We took along several bottles of donated breast milk in a cooler, as well as an ice pack. At security, they asked to open up our cooler as usual. All seemed normal. And then came the question, "But how old is your baby?"
"He's thirteen months."
"Oh, ok. This is fine. Go ahead."
The exchange seemed simple enough, but suddenly left me wondering, is there an age at which I won't be able to bring milk along for my baby? Is thirteen months ok, but say, eighteen months too old? Why did they ask my baby's age?
We rely upon donated breast milk to feed our baby. I nurse him using an at-breast supplementation system, and am able to enjoy a satisfying breastfeeding relationship as a result. I would like to keep breastfeeding my child as long as he needs it. Since the World Health Organization recommends breastfeeding for two years AND BEYOND, I am and will continue to be grateful for human milk donations. If and when we are no longer able to find donated human milk, we will probably move to using whole goat's milk in the supplementation system. Goat's milk is closer to human milk than cow's milk is, but it is probably not commonly available beyond airport security.
During our stay in Vancouver, I looked up the rules. In Canada, you may only bring extra liquid aboard a flight for a child UNDER the age of 2. So, I decided to start a petition on change.org. Please sign it and share widely!
http://www.change.org/petitions/canadian-air-transport-security-authority-ease-restrictions-on-breast-milk-in-carry-on-baggage#
"Canadian parents using expressed breast milk currently face greater restrictions when flying with their children than do their American counterparts. Only passengers traveling with infants UNDER the age of 24 months may bring aboard more than 100ml of liquid per container, inside a 1 litre plastic bag. Women traveling without their babies are not permitted to bring their expressed milk on board. Those traveling with children above age two are not exempt from restrictions on liquids.
"The World Health Organization recommends breastfeeding until age 2 AND BEYOND. For those parents who must express their milk and bottlefeed, or who use donated milk and an at-breast supplemental nursing system, carrying liquid on their persons is a must. Why should the Canadian Air Transport Security Authority decide at what age a child no longer needs breast milk, especially during potentially stressful travel?
"Passengers traveling without their babies should also be allowed to carry their precious breast milk rather than pump and dump. Breast milk, known in the birth world as "liquid gold" for its important health benefits, should be exempt from the usual restrictions on liquids.
"In the US, breast milk is treated as liquid medication and passengers may carry it on board in quantities greater than 3 ounces WITH OR WITHOUT A BABY OR TODDLER PRESENT. Sign this petition and tell the Canadian Air Transport Security Authority to start valuing breast milk as vitally important nutrition for babies and children!"
http://www.change.org/petitions/canadian-air-transport-security-authority-ease-restrictions-on-breast-milk-in-carry-on-baggage#
5 May 2012
Night Weaning, and Why We're Not Ready for it
This Mom went on to describe her reasons for night-weaning her youngest child and how difficult it had been. She had to go back to work and was simply exhausted from being woken up frequently to nurse at night. Sounds familiar to many of us, I'm sure. "The first night he cried for five hours. My husband had me wear head phones so that I could get through it. The next night he only cried for about three hours. Pretty soon we got down to ten minutes."
Since embarking on this mysterious and beautiful parenting journey, I have come to understand why sleep deprivation can be used as a torture technique. It genuinely feels horrid. I have been known to say when I'm getting to an extreme of exhaustion, "I want to die I'm so tired!!"
But I also cannot picture night-weaning anytime soon, so I guess it's all the more fortunate that I do not yet have to go back to work. Jacob just turned one, and he is going through an extraordinary developmental stage that is demanding for everyone involved. Frankly, he thinks he is too busy to nurse much during the day, and I believe him! He is learning to walk, to climb stairs (though not to go back down them), to eat solid foods, to share toys, and to cope with strong emotions. And he will soon surpass his dads in his confident use of electronics. During the daytime he is rushing to grow up, which leaves only the nights for being a baby with an intense need for both human milk and touch.
I understand why people night-wean their kids, and I don't blame them for wanting to do it. But I think about my poor little guy trying so very hard to explore and establish his independence in his waking hours, and I know that now is definitely not the time for us. If it is painful for me as an adult to lose sleep, I am sure it would be even more so for him to go without the comfort of nursing while he attempts to process the huge adventures of his days. It is hard work to be a baby.
As my many attachment-minded friends love to remind me, we will get through it, and this too shall pass.
4 Apr 2012
Responsive Parenting
 | ||
| My infant doesn't know I'm transgender. |
What does my baby know? He feels that he wants to be held a lot, although this is beginning to change as he explores the world more and more. He knows that when he nurses, much of his body touches a warm, caring adult body and he is safe. He feels that he wants to suck, A LOT.
So I have to respond selectively to the people around me, which is not always easy. I'm ultra-sensitive to my boy. I try to breastfeed him when he gives early signs that he may want to nurse. I am insensitive to the man in the restaurant who is staring as I latch on my little guy. If I'm feeling brave, I look up and smile at him, but mostly I pay attention to positioning my baby and the SNS. I don't respond to the woman who stares at me or the teenagers who point and giggle. I'm busy. If these other folks are hungry, I'm pretty sure they can go off and find their own food without my help, but my baby is depending on me. He trusts me.
I will always remember the funny looks I've received, while my baby may or may not remember breastfeeding depending on his age when we stop. But he will get through his toddlerhood and early childhood with a strong sense of attachment. He knows that I will always respond.
This post is part of the Attachment Parenting is for Everyone blog carnival, hosted by Attachment Parenting International. Learn more by visiting API Speaks, the blog of Attachment Parenting International.
13 Jan 2012
Nursing in Public
Today I fed Jacob immediately before leaving home for the walk-in clinic down the street, but after forty-five minutes of waiting perfectly quietly, he started to get antsy. I struck up a conversation with the woman sitting across from me, distracting him and biding myself some time. She mentioned that she has twin baby boys, seven months old. We compared notes for a while, and she said she breastfed them until six months and then gave up out of sheer exhaustion. I applauded her effort, congratulating her on breastfeeding through a very important period in her sons' lives.
Then she mentioned that she always pumped for them. I commiserated, "Oh, that is difficult. Were they born premature?"
"No, they got to full term. 37 weeks to the day."
"That's fantastic! Great job." But I was still wondering. "Did they have trouble latching then?"
"No, I never tried. It's the same way I did it with the first one. I just pumped. That way somebody else can do the feedings too. It takes so much time to pump though."
Bizarre! She thought it was easier to pump than to breastfeed, so that somebody else could feed them too? What about getting up to do the pumping, getting up to feed the babies, cleaning the pumping equipment, cleaning the bottles? And to miss the closeness of a breastfeeding relationship! I guess she never considered doing some feeding at the breast and then pumping some so that her husband could feed the boys. I am so sorry for this woman - I don't think she knows what she missed.
Anyway, soon enough Jacob just had to eat, so I fed him. Right there. About two feet away from old ladies, and young ladies, and scruffy men, and big fat men, and the receptionists. And they mostly frowned and looked away. The ones who had been smiling at Jacob before didn't smile at him anymore once we were done nursing. But none of them dared say anything. I love it. If anyone questioned what I was doing, I planned to ask if they would prefer for him to cry, for the pleasure of the whole waiting room. One way or another, we will assault your senses, either visual or auditory. It is much easier to look the other way than to shut off your ears. I suppose they figured as much.
A friendly new woman came in, who hadn't seen me breastfeeding. She asked how old he was. I told her, and she mentioned she has a six month old. I told her we had a trip coming up and I was wondering how to make it go smoothly for my little boo.
"Oh, make sure you get onto the plane with him on an empty stomach because he'll need to drink a whole bottle on the way up and a whole one on the way down to help his ears adjust to the pressure changes."
"He's still breastfed. We'll make sure he eats."
"Wow, really? Still breastfed? Mined weaned herself at four months."
How does a baby wean herself at four months? Did she really decide to commit suicide? Stop eating her available liquid food before she would be able to chew and swallow even rather soft solid foods? I can't imagine an infant so young having a death wish like that. I know that somehow there was a communication failure, but I'm sure that this baby didn't want to wean herself.
When I got in to see the doctor, he tried very hard to be respectful. "Well, hello Dad! How are you today?" He looked at the chart. "I mean, Mom!! How are you?"
"No, it's Dad," I said.
"But why does your chart have an F on it?"
Here we go again, I thought. "Because I'm transgendered. I was born female, transitioned to male by taking hormones. I identify as male. But my birth province won't change my ID unless I get a complete ovariohysterectomy. It sucks."
"Well, would you like me to change it in your file here?"
I thought about this for a minute. It was a kind offer.
"No, probably better not, because my government health card still says F. It would mess up your system and they'd likely decide I'm not insured or something."
He nodded sympathetically. "So, what's up?" And we got down to business.